The psychoactive class of drugs known as Benzodiazepines was discovered by a Polish-American chemist in 1955. As an anti-anxiety drug, Benzos, as they’re often referred to, have a wide range of medical applications. These highly addictive drugs are, in fact, so effective that by 1977 they became the most prescribed medications in the world.
 The American Psychological Association (APA) reports that 11 to 15 percent of all adults have used benzodiazepines in the last year. Individuals prescribed or abusing benzos will develop a tolerance to the medication, and must ingest more to feel the same effects, which can lead to addiction. Physical and psychological dependence can develop in one to two months, and even faster at high dosages.
The American Psychological Association (APA) reports that 11 to 15 percent of all adults have used benzodiazepines in the last year. Individuals prescribed or abusing benzos will develop a tolerance to the medication, and must ingest more to feel the same effects, which can lead to addiction. Physical and psychological dependence can develop in one to two months, and even faster at high dosages.
Used for both physical and mental conditions, such as panic attacks or nausea and vomiting, benzos calm or slow down nerves in the brain.
What are Benzodiazepines Used For?
- Anxiety Disorders – Valium, Ativan, Xanax, Klonopin
- Alcohol Withdrawal – Librium
- Seizures – Klonopin, Tranxene, Valium
- Insomnia – Doral, Restoril, Halcion
- Muscle Relaxation – Valium
- Anesthesia – Ativan, Valium
Benzodiazepines attach themselves to receptors in the brain called GABA neurotransmitters. Research has shown that GABA is responsible for controlling fear and anxiety. This reaction in the central nervous system causes sedation, anxiety reduction and muscle relaxation.
Data suggests that 80 percent of benzodiazepine abuse is done in combination with other drugs, most commonly opioids, like heroin and methadone. Teenagers are more likely to abuse marijuana and benzodiazepines, while adults over the age of 45 abuse the drugs along with alcohol.
The misuse of benzos can be deadly. Taken in combination with stimulants, such as alcohol, or with opioids, both the heart and the cardiovascular system can be slowed or stopped resulting in a coma maybe even a fatal overdose. Mixed with prescription muscle relaxers, benzodiazepines can also damage liver and kidney function.
Withdrawal from benzodiazepines can result in painful symptoms, such as the return of anxiety, insomnia and sensory hypersensitivity. In the case of long-term abuse and addiction, withdrawal can be more severe. Specialists have noted a protracted withdrawal syndrome with depression, anxiety and insomnia lasting months at a time, even after a patient has stopped abusing benzos.
A physician should oversee treatment for benzodiazepine addiction. The National Institute of Health suggests that patients should be slowly tapered off the medication in an effort to ease withdrawal symptoms, and not taken off “cold turkey.” In addition to a gradual dosage reduction, psychological support in the form of therapy, in-patient or outpatient treatment is effective. In rehab, patients and their doctors can address any other issues, such as alcohol abuse, opiate addiction and any underlying mental illness.
In many cases, people prescribed benzodiazepines can unwittingly become dependent through no fault of their own. It’s important to remember that addiction is a disease and must be treated. Learning new strategies and coping mechanisms to deal with the stress and anxiety of day-to-day life will lead individuals to a longer last recovery.
The infographic below illustrates some of the uses and abuses of benzodiazepines.
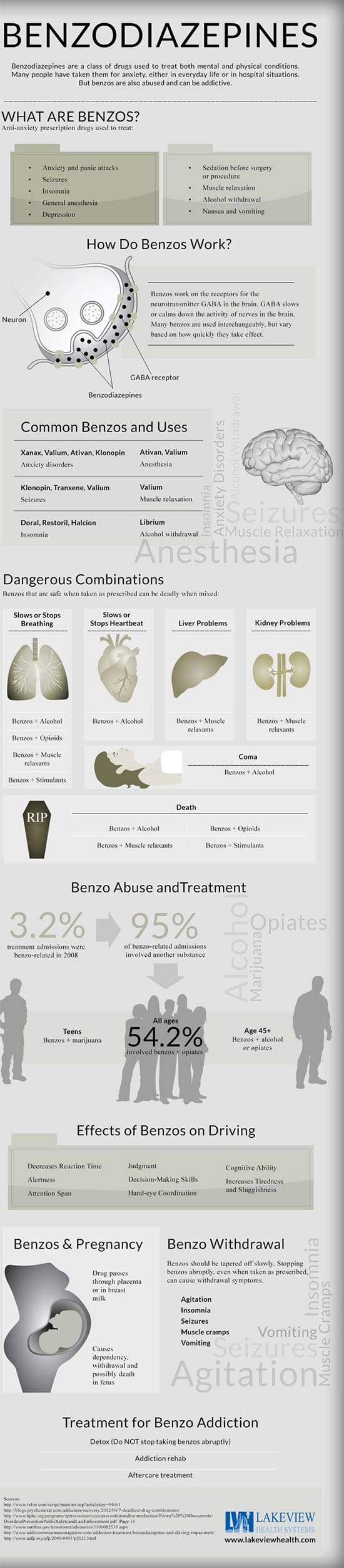
To see a larger version of this infographic visit the visual.ly website.
Related:
What are the Withdrawal Symptoms of Benzodiazepines?
Baby Boomers and Senior Substance Abuse Addiction
Will Electronic Prescriptions of Controlled Substances Deter Fraud?





