The Food and Drug Administration (FDA) recommended making certain prescription painkillers more difficult to obtain in October 2013. Opioid drugs like Vicodin, which are based on Hydrocodone, would be reclassified as Schedule II drugs and would not be automatically refilled.
As pain medication abuse increases across the country, the announcement was expected. At the same time, the FDA approved the use of a new drug, Zohydro (hydrocodone bitartrate), despite warnings from critics, creating a backlash in the media.
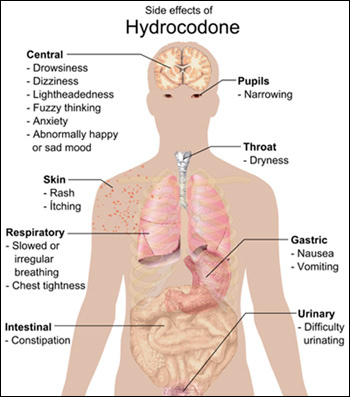 Hydrocodone Side Effects Image courtesy of Mikael Häggström
Hydrocodone Side Effects Image courtesy of Mikael Häggström
One of the main problems with Zohydro is the ease with which it can be crushed and taken in ways not intended. This opens the door for widespread misuse, complicating the already enormous problem of opioid abuse.
In December 2013, the attorney general from 28 states went to the FDA to advise against approving the Zohydro because it offers “5 to 10 times more heroin-like narcotic than traditional hydrocodone products.”
Wanting to get a better idea of the problems this might cause, we talked with , about Zohydro and opiate abuse.
What do you think of the FDA’s decision to approve the opioid, Zohydro, without built-in deterrents for abuse?
It’s unfortunate that while the FDA is rescheduling Hydrocodone, a drug like Zohydro will be FDA approved without any built-in deterrent formulation. This medication can be diverted, easily crushed, and be used by other routes such as IV with potentially dangerous overdose and death.
However, the FDA needs to follow its own policies and regulations. I believe that’s the case for this drug, which was under development for a long time and got approved using a loophole in the policy.
Do you think having another opioid on the market will cause another increasing prescription drug abuse? Why or why not?
Zohydro falls under new scheduling and regulation of ER/LA (Extended-Release/Long-Acting) opioid guidelines. Where Physicians get training and a follow-up study should be ongoing by Pharma company to monitor misuse, overdose, and death. It may have some impact on increasing opioid abuse but the jury is still out.
Do you think specific seasons impact opioid abuse/dependence (winter, holiday season) – do you think it’s more prevalent during certain times of the year, or not?
There is no evidence to suggest that opioid use disorder is seasonal because once someone is dependent on it, it’s very hard to stop. Withdrawal symptoms are excruciating and because of the fear of withdrawal symptoms, patients continue to use them until they seek professional help to stop using opioids.
Recreationally, some people may use it on occasion or during the holidays but that’s just misuse not dependence, however, it can lead to full-blown dependence if continued for an extended period of time.
What are the main signs/symptoms of opioid abuse in women to look out for?
Usually, they become sleepy and not alert, have slurred speech, are possibly constipated, and have constricted or pinpoint pupils. These are the main sign and symptoms to look for.
What are some ways to help prevent opioid abuse/dependence? What are steps to take if someone thinks they are dependent on/abusing opioids?
1. Anyone who has been prescribed opioids needs to be educated about the potential for tolerance, withdrawal symptoms, abuse, and dependence. Ongoing monitoring and a clear exit strategy should be in place, and the prescribing physician should do a periodic assessment.
It’s important to remember, if someone has a family history of Addiction, they need to take precautions while using opiates, inform their physician about any possible family history, and terminate treatment with opiates within the indicated period. Family or primary support involvement in treatment is helpful.
People with a family history should also refrain from experimenting with opiates or any other mind-altering drugs.
2. If someone is taking opioids beyond the intended period of time and their family is concerned, they should notify the treating physician as soon as possible. They also need to have an open discussion with the patient taking the opioids and offer help with treatment whenever necessary.
3. If a person continues to abuse any medications and is not ready to change, the family should engage with the person and continue encouraging them to seek help until the patient complies. In some cases, professional intervention may be appropriate.
4. If someone realizes that they are abusing or have become dependent on opioids, they are 50% on their way to treatment, meaning they are ready to change and seek help. They should immediately seek professional help, starting with medical detox and continuing with ongoing treatment.
Related:
Opioid Deaths Decrease Life Expectancy Rates (2nd Year in a Row)
10 Ways to Treat Pain Without Opioids or Prescription Painkillers





