In late October, President Trump spoke about how his brother, Fred Trump Jr., battled alcoholism and died an early death, at 43 years old. In the same speech, the president declared the crisis of opioid overdose deaths and addiction a federal public-health emergency.
What Happens by Declaring a Public Health Emergency?
The Public Health Emergency Act allows government agencies to shift a certain amount of money around to address the opioid crisis.
However, some experts like physician Susan Blumenthal, think that comes with some caveats. The former assistant surgeon general and a retired rear admiral in the U.S. public-health service, points out that the needed funds are likely going to be removed from other vital public-health programs.
“The action allows for shifting of resources within HIV-AIDS programs to help people eligible for those programs receive substance abuse treatment, which is important. I’m not sure how that happened, but we still have an HIV epidemic in America,” Blumenthal told Washington Post contributor Jonathan Capehart on his podcast, Cape Up.
Amid the chaos in U.S. politics right now and the ever changing 24-hour cable news cycle, it’s easy to lose sight of just how drastic a toll the opioid crisis is having on the country.
How Bad is the Opioid Epidemic?
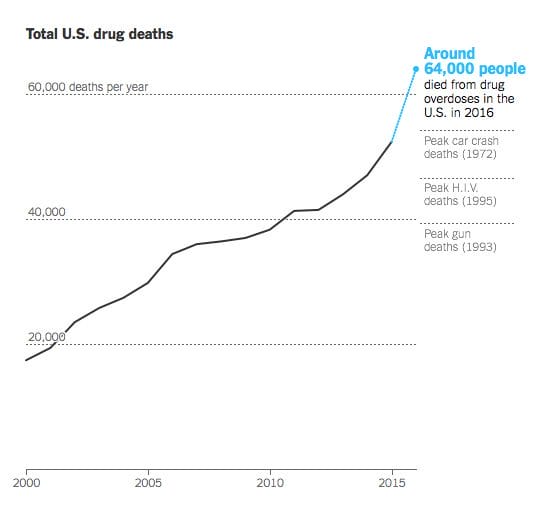
This New York Times graphic (below) published in September shows just how deadly the epidemic is, becoming the leading cause of preventable deaths for all Americans under the age of 50.
The spike in fatal overdoses is largely a result of heroin laced with the synthetic opioid fentanyl, which is so toxic that handling it without gloves can be lethal.
Most Americans dying from heroin overdoses didn’t start using heroin until after they became addicted to prescription painkillers, prescribed to them by their physicians.
There’s new evidence, though, that as heroin has become more available, a greater number of people are getting addicted to that substance first.
How Has Opioid Addiction Changed in the Past Ten Years?
“In 2005, 80 percent of people who were dependent on opioids started with painkillers and 10 percent started with heroin,” says Vox policy reporter Dylan Scott on a podcast called The Weeds. “In 2015, that had shifted to about 50 percent of people starting with painkillers and 33 percent starting with heroin.”
This is an even bigger wrench in the opioid public-health emergency because lawmakers in Washington are mostly focused on prescription medicines that lead to addiction.
By Blumenthal’s estimation, the government needs to dedicate some $45 billion, at minimum, to properly address the opioid crisis. She admits, though, that she’s worried about where that money would come from. Blumenthal’s also concerned that executive orders gutting the Affordable Care Act (ACA/Obamacare) will make treatment even more difficult to access and afford.
“Three out of 10 people getting addiction services are on Medicaid and 31 states and the District of Columbia did expand Medicaid,” she told Capehart. “The main point here is to underscore we need comprehensive insurance access because these are not issues that can be viewed by themselves but in an integrated way.”
Whether or not the government’s capable of handling this growing disaster is yet to be seen, but for many healthcare professionals, calling it a public-health emergency is not the solution.
Related:
Study Shows Rise in Pediatric Opioid Poisonings and Deaths
The Dangers of Unknown Dosage Strength, Shared Needles, and Impurity
Ten of the Biggest Addiction Myths